Presentation:
Signalment: 10-year-old female spayed mixed breed canine
History: Prior history of hypothyroidism and osteoarthritis. Presented for evaluation due to decreased appetite, increased water intake, and regurgitation.
Physical findings: Slightly increased respiratory rate and effort, mildly distended abdomen, suspected hepatomegaly on abdominal palpation.
CBC/Chemistry: Elevated liver enzymes (ALP = 1173, ALT = 674), mild hyperbilirubinemia (1.3), severe neutrophilic leukocytosis (wbc = 37.31k, neut = 34.88k), platelets = 48K, cPLI = 650, T4 mildly elevated (5.4).
AFAST: Organized bile within the gallbladder, supportive of biliary mucocele.
Initial Treatment:
The patient was hospitalized for supportive care and monitoring. Treatment included intravenous fluids, cefazolin q 8 hours, enrofloxacin q 24 hours, Cerenia q 24 hours, and Galliprant q 24 hours. After 48 hours of treatment, the patient was noted to be inappetent, and abdominal pain persisted. Serial labwork revealed progressive increase in total bilirubin (6.6) and ALP (unreadable), worsening neutrophilic leukocytosis (wbc = 42.52k, neuts = 37.13k), platelets = 370k. Full abdominal US was recommended. Thoracic radiographs were unremarkable.
Abdominal Ultrasound Findings:
Gallbladder and Common Bile Duct (CBD)
The gallbladder appears moderately enlarged. The wall appears thickened and heteroechoic. The lumen contains a moderate/marked amount of organized echogenic debris that is suspended centrally within the lumen. Linear echogenic striations emanate from the central debris to the wall. The proximal common bile duct is mildly dilated (4mm) with anechoic lumen; distally, the duct is obscured by overlying GI gas.
Other
The tissue surrounding the apex of the gallbladder is hyperechoic. There is scant anechoic peritoneal effusion (sampling not feasible) scattered throughout the abdomen.
Diagnosis:
1. Biliary mucocele, mature with probable rupture
2. Ascites, scant
3. Hepatopathy
4. Pancreatitis
5. Severe neutrophilic leukocytosis—r/o inflammation vs. infection
6. Hypothyroidism
Surgical Findings:
The morning following the ultrasound, abdominal exploratory surgery was performed. Intraoperatively, generalized bile peritonitis was present. The gallbladder was markedly enlarged and firm, with a large rupture along the border of the ventral aspect of the quadrate lobe. The liver was mildly rounded in contour, with focal areas of fibrin on the surface. The common bile duct could not be visualized due to thickened, inflamed mesenteric fat. An enterotomy was performed, and a red rubber catheter passed easily into the CBD. No bile could be aspirated, but the CBD flushed without resistance, confirming patency. Cholecystectomy, liver and gallbladder biopsy, and liver and bile culture were performed.
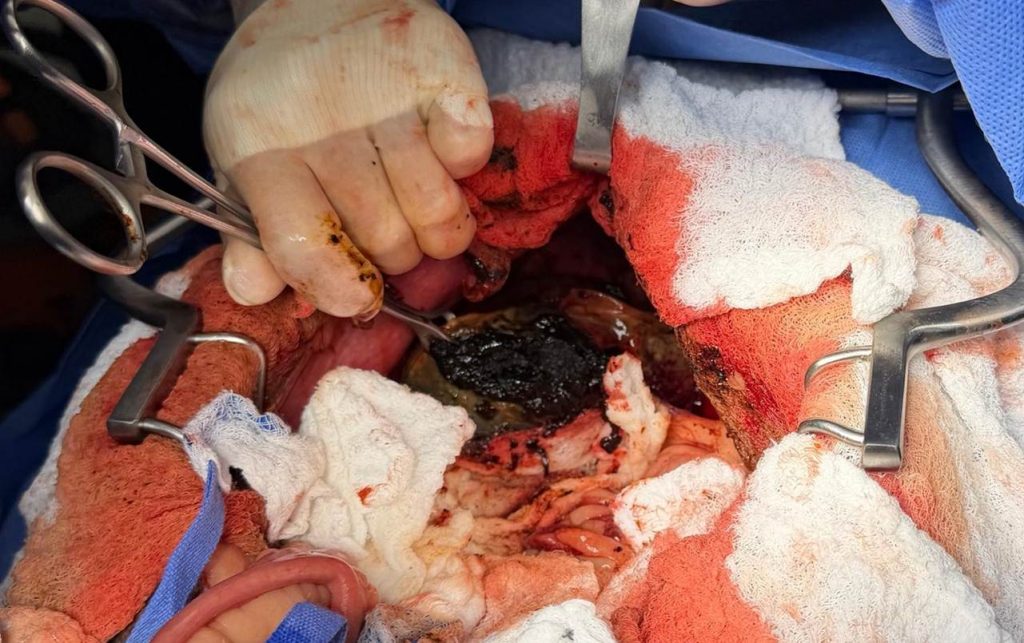
| Outline of gallbladder with organized bile visible at rupture site |
Adapted from: Diagnosis and management of gallbladder mucocele formation in dogs; J Am Vet Med Assoc. 2025 Mar 19;263(6):777-785.
Case Follow-Up:
The patient remained hospitalized for supportive care for 3 days and was then transitioned to outpatient care. The day following surgery, total bilirubin had only improved mildly, but strength was slightly increased. At 48 hours postoperative, she was willing to eat small amounts for the owner. Steroid therapy was initiated to address ongoing inflammation. At 72 hours, total bilirubin had increased back to 6.2, and wbc increased to 53k, but she remained stable, continued to have a mild appetite, and was afebrile. Steroid therapy was continued, and ursodiol was added. After strength and appetite improved gradually. However, despite clinical improvement, her total bilirubin was still significantly elevated (5.0) six days following surgery. Histopathology confirmed a biliary mucocele and moderate, diffuse, chronic cholangiohepatitis. The patient’s ongoing care will be focused on managing her hepatic disease.
Decision-Making In Biliary Surgery:
Onset of clinical signs secondary to extrahepatic biliary obstruction is often acute, but chronic presentations do occur. Given the progressive lab changes and concern for gross rupture in this case, there was a clear indication for urgent surgical intervention. There are limited reports of biliary mucoceles resolving with medical management, including some dogs treated for concurrent predisposing endocrinopathies (hyperadrenocorticism, hypothyroidism). However, evidence suggests that surgical treatment improves outcomes. Even when gross evidence of rupture is not present, 70-80% of mucoceles exhibit mural necrosis histologically. In the rare case of obstructing cholelithiasis, stones will continue to form if the gallbladder is not removed. Thus, cholecystectomy is indicated in the vast majority of these cases.
Confirming CBD patency is a must…
Because of the shared outflow of the cystic and hepatic ducts, it is crucial to confirm the patency of the CBD prior to cholecystectomy. If patency cannot be established, cholecystectomy will result in death. When the CBD is not dilated and total bilirubin is normal, manual gallbladder expression may be considered. When the CBD is dilated or when clinical obstruction is evident, catheterization and flushing of the duct is necessary. This allows for confirmation of patency and removal of residual organized bile or stones, thus reducing the risk of persistent obstruction.
What if the CBD is not patent?
If the patency of the CBD cannot be established, biliary diversion would technically be necessary to allow for restoration of hepatic bile flow. However, in my experience, the gallbladder wall is often not healthy enough in mucocele cases to use for diversion. Thus, intraoperative euthanasia can become necessary. Diversion is often more reasonable in cases of pancreatic disease resulting in obstruction, but it should be communicated that associated complication rates are high. Choledochal stenting may also be used to temporarily improve signs while concurrent pancreatic disease is treated (pancreatitis, pancreatic abscess, etc.). Successful medical management of the inciting pancreatic disease remains the priority, given that the prognosis for patients who require surgery to help treat advanced pancreatic disease is poor.
Other considerations:
One of my mentors always said, “Gallbladders require a little bit of surgery and A LOT of medicine.” We all know that surgery is only a part of the solution when managing biliary obstruction. These patients should be screened for concurrent pancreatitis, coagulopathy, and sepsis, and stabilized prior to surgery (when possible). Perioperatively, they can be critical, with 74% experiencing hypotension during treatment in one study. Postoperatively, continued monitoring and management of these factors, as well as treatment of existing hepatopathy (acute vs. chronic), is imperative to maximize the chance of survival. Thus, some of these cases benefit from referral to a critical care and/or internal medicine specialist.
Surgical Outcomes In The Literature:
Mortality rate associated with cholecystectomy for biliary mucoceles in dogs with clinical signs is significant, ranging from 17-40%. More recent studies suggest that outcomes are more favorable when biliary mucoceles are treated on an elective basis. Average mortality for asymptomatic dogs when surgery was performed electively was 5%, versus 20% for those clinical patients treated emergently. Gross gallbladder rupture increases the risk of mortality by 2.7 times. Other factors that increase mortality include pancreatitis, coagulopathy, sepsis, azotemia, hyperadrenocorticism, and increasing patient age. Most mortalities occur within 2 weeks of surgery.
Surveillance And Client Education Are Key:
When biliary disease is suspected, early identification improves successful management. I lean on the internists to determine when medical management may be a reasonable approach for early mucoceles. Regular follow-up is still prudent to identify progressive disease in these cases. It also benefits the patient and clinician greatly to invest the time to convey the complex nature of biliary obstruction and hepatic disease to owners. Although risks must be weighed for each case, early surgical intervention has been shown to improve long-term outcomes for many dogs. Even in initially stable cases, the owner must be aware of the risk and clinical sequelae of obstruction and rupture. In emergent cases, the owner should be appropriately prepared for intraoperative and postoperative complications, to guide decision-making when complications arise.
Relevant Review Articles:
Diagnosis and management of gallbladder mucocele formation in dogs
JL Gookin, KG Mathews, G Seiler
J Am Vet Med Assoc. 2025 Mar 19;263(6):777-785.
Gallbladder mucocoele: A review
TM Smalle, AK Cahalane, LS Köster
J S Afr Vet Assoc. 2015 Dec 9;86(1):1318.
